Gentle Reader,
Sciatica, sciatica, sciatica. On every hand I hear people complaining about sciatic pain, drop foot, back difficulties and arthritis in general. I have had more acute sciatic pain plus a long stretch of time at home (no travel plans until July) so I decided to try cortisone for sciatica. I first focussed on discovering the cause. What would a medically trained physician have to say about my condition?
I imagine most people begin in the doctor’s office. You, who read my posts, may be among those who seek alternative care first. I have done Feldenkrais, Deep tissue sports massage, private pilates, Myofascial Release, Raiki, Alexander, Therapeutic Yoga, chiropractic, Physical Therapy—what am I forgetting? Ah, yes, my wonderful team at the Xgym, half the time and twice the results. Personal trainers who tailor my 25 minute workout to build upper body, leg and core strength while protecting my back.
My first injury happened in 1989 with a major exacerbation in 1992. Back then I did all the above and my doctor of choice was Stan Herring, a neurosurgeon who now limits his practice to the University of Washington Huskies and the Sea Hawks. He’s the doctor who looked at my x-rays and a later MRI and asked if I’d come in a wheelchair. “Get strong, Betsy. Your bones are no good for surgery so get strong.”
If you know me and see me on Face book, you know that is exactly what I have been doing. Weekly hiking, daily walking up and down the hills of West Seattle, long walks in exotic places in the off season, cross country skiing and snow shoeing when we have snow in our Cascades.
The sciatic has gotten progressively worse affecting my right leg and causing numbness and sometimes extreme pain. I put myself under the care of Dr. Ren at the Polyclinic. She is a physical medicine doctor who specializes in keeping people moving who suffer from back related problems (among other things). She confirmed that I have extreme spinal stenosis and osteoarthritis, two herniated disks at L4 and L5. She sent me to physical therapy for eight session. As has been true with previous visits to PT’s, I had fun with those young specialists and enjoyed their stretching, icing and exercises, but nothing beneficial came of it. In fact, the gross motor activities prescribed may have made my condition worse.
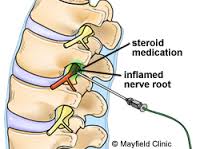
Next step was to get the shot of cortisone for sciatica in the L5 area where the narrowing is so small, it’s a wonder any nerve impulses get through at all. I’ve been scheduled for this procedure three previous times and canceled each time. I wasn’t ready. Dr. Ren did a fabulous job. Her needle found the spot producing an electric shock that sprung my leg all the way to my two middle toes to life with a jerk. After I caught my breath, I congratulated her.
The first day I felt wonderful and so moved stuff around in the garage. Stupid. Without the pain, I realized my gait was completely cattywampus—right hip collapsing with each step, left leg struggling to hold me up. Something whispered to me, “Go back to Becci Parsons and let her healing hands remind you how to stand and walk and sit and roll over.” Becci is the Feldenkrais therapist who got me back on my feet after the herniation so many years ago. She is a former dancer and has the same “keep moving” spirit I have. She has suffered from a similar herniation and has ended up with surgery. She can move fluidly with nearly equal strength on both sides (her right side has some weakness and lack of nerve response when her foot gets caught).
Becci, after three session, has me sitting on my sits bones with a nature curve in my lower spine, pressing one heal to the floor on the exhaling breath while lifting the right heal ever so slightly. I am paying attention to the distance between my arm pit and my hips on both sides, keeping that distance equal. I am paying attention to every muscle group that tries to help lift that right heal. Tiny movements with laser focus to re-pattern the injured nerves and muscles. She checked out my gait with the hiking sticks and said it was remarkable how my shoulders remained even, my right side did not collapse and my left hip didn’t swing out. That decision on my part to walk everywhere with hiking sticks was the best self care for my condition. It gets me a seat on a crowded bus, too.
I have an appointment for a new MRI although Dr. Ren’s assistant Diana didn’t see how the stenosis could have gotten any worse. Then I will have a surgery consultation with Becci’s neurosurgeon. I hope I don’t have to go there, but I am willing if it would help me gain real strength on my right side.

The blessing is not being in pain. I stopped taking Shaklee’s Pain Relief Complex which inhibit the pain path without any side effects. Low and behold, other arthritis pain showed up in my hands. I don’t hike as far as the other members of my gang of hikers, but I am strong enough to lead the pack and am pain free. My hiking friends have been solicitous, gradually increasing the length and the elevation gain. Last week and next will be 700 ft of altitude gain and six miles round trip (Boulder Creek trail of Hwy 530). I know it well and there are places to stop if I need to let the others go on.
There is something about spending a day in the wilderness every week that keeps my spirit soaring and my sense of well being strong. I’ve mentioned before that our gang has scouted out wheel chair accessible wilderness walks for that time in the future when one of us can’t walk. So far, I don’t need to be pushed.
I share my pain, suffering and healing stories in case they resonate with something you are going through, or someone you know. If you have any interest in connecting with any of the practitioners I have used, please follow the hot links to them. If you are interested in trying the supplements and dietary changes that have been so helpful to me, please check out this post in particular. If you have questions or comments from your own experience, I and my readers would love to hear from you.
Thanks for reading,
Be well, Do well and Keep Moving,
Betsy
206 933 1889



